What Causes Vein Disease? Understanding Chronic Venous Insufficiency in St. Louis
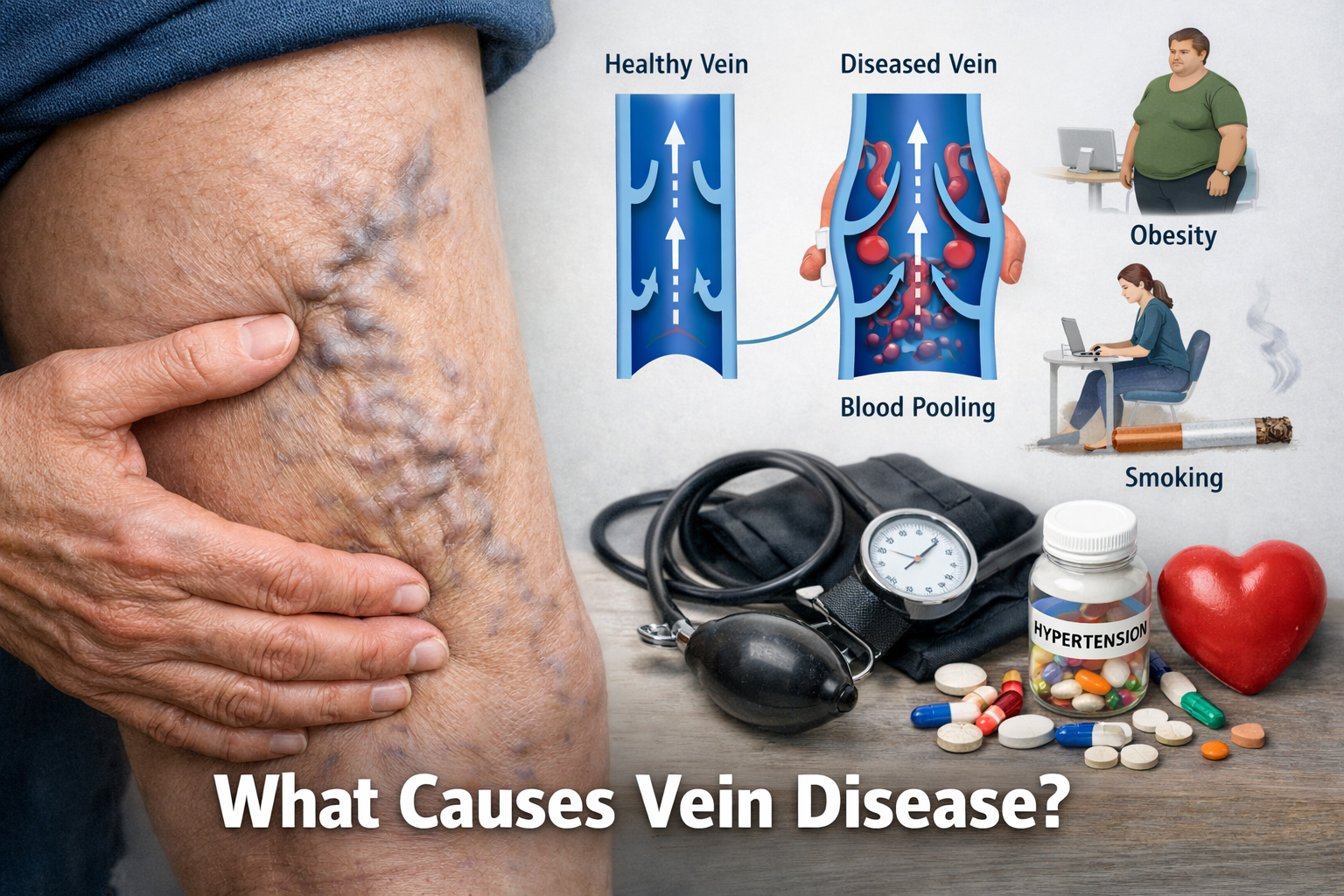
What Causes Vein Disease? Understanding Chronic Venous Insufficiency
Vein disease is far more common than most people realize. Millions of Americans experience symptoms related to poor venous circulation, yet many assume that visible veins or leg discomfort are simply cosmetic concerns or a normal part of aging.
In reality, vein disease is a circulatory condition that can progressively worsen if not properly evaluated and treated.
At Sheen Vein, we regularly work with patients throughout St. Louis, Clayton, Chesterfield, Arnold, and Farmington, Missouri who are experiencing symptoms such as leg swelling, heaviness, restless legs, or visible varicose veins. These symptoms often indicate a condition known as chronic venous insufficiency (CVI).
Understanding what causes vein disease is the first step toward recognizing symptoms and improving vascular health.
In this article we will explore:
- What vein disease is
- Why it develops
- Risk factors that contribute to it
- Symptoms that patients often experience
- Why early diagnosis and treatment matter
What Is Vein Disease?
Vein disease, often referred to as chronic venous insufficiency, occurs when the veins in the legs struggle to return blood back to the heart efficiently.
Healthy veins contain small one-way valves that help blood travel upward toward the heart against gravity. These valves open to allow blood to move forward and close to prevent it from flowing backward.
When these valves become weakened or damaged, blood may begin to pool in the veins of the legs.
This leads to increased pressure in the veins and the development of symptoms associated with venous disease.
The Mayo Clinic describes chronic venous insufficiency as a condition in which the leg veins cannot properly return blood to the heart, often resulting in swelling, varicose veins, and skin changes.
https://www.mayoclinic.org/diseases-conditions/chronic-venous-insufficiency/symptoms-causes/syc-20352524
Similarly, the Cleveland Clinic explains that chronic venous insufficiency occurs when vein valves become damaged or weakened, allowing blood to flow backward and accumulate in the legs.
https://my.clevelandclinic.org/health/diseases/16872-chronic-venous-insufficiency
Why Veins in the Legs Are Vulnerable
The veins in the legs face a unique challenge compared to veins elsewhere in the body.
Blood must travel upward against gravity from the legs to reach the heart.
This process relies on several mechanisms:
- functioning vein valves
- contraction of leg muscles
- normal vein wall structure
If any of these mechanisms become impaired, venous circulation may become compromised.
Over time, this can lead to venous hypertension, which is increased pressure within the veins.
This pressure can cause veins to enlarge, twist, and become visible under the skin.
Common Causes of Vein Disease
Vein disease usually develops gradually over time and is influenced by several factors.
Understanding these causes can help explain why some individuals develop venous problems while others do not.
1. Genetics
Genetics is one of the strongest risk factors for vein disease.
If one or both parents have varicose veins or chronic venous insufficiency, there is a significantly increased likelihood that their children may develop similar issues.
Inherited factors may include:
- weaker vein walls
- less effective vein valves
- connective tissue differences
These inherited characteristics can make the veins more susceptible to valve dysfunction.
2. Aging
As people age, the structure of veins and connective tissues gradually changes.
Over time:
- vein walls may lose elasticity
- valves may weaken
- circulation may slow
These changes can make it more difficult for veins to maintain proper blood flow.
This is why vein disease often becomes more noticeable after the age of 40.
3. Prolonged Standing or Sitting
Occupations that involve long periods of standing or sitting can place significant stress on the venous system.
Examples include:
- healthcare workers
- teachers
- retail employees
- office workers
- factory workers
When the legs remain in the same position for long periods, the calf muscles do not actively assist circulation.
This can cause blood to accumulate in the lower legs.
Over time, increased venous pressure may weaken vein valves.
4. Pregnancy
Pregnancy places additional stress on the venous system.
Several factors contribute to vein disease during pregnancy:
- increased blood volume
- hormonal changes that relax vein walls
- pressure from the growing uterus on pelvic veins
These changes may slow blood flow from the legs back to the heart.
Although some pregnancy-related vein issues improve after delivery, others may persist.
5. Obesity
Excess body weight can increase pressure within the veins of the legs.
This additional pressure may strain vein valves and contribute to venous dysfunction.
Obesity is also associated with reduced physical activity, which may further impair circulation.
6. Lack of Physical Activity
Movement plays an important role in venous circulation.
When the calf muscles contract during walking or exercise, they act as a “muscle pump” that helps push blood upward toward the heart.
A sedentary lifestyle may reduce this pumping action.
As a result, blood may pool in the lower legs.
7. Previous Blood Clots
A history of deep vein thrombosis (DVT) can damage vein valves.
When a clot forms inside a vein, it may stretch or injure the valve structures.
Even after the clot resolves, the affected valves may not function properly.
This condition is sometimes referred to as post-thrombotic syndrome.
8. Hormonal Influences
Hormones can influence vein structure and elasticity.
For example, estrogen and progesterone can relax the walls of veins.
Hormonal fluctuations related to:
- pregnancy
- birth control
- hormone therapy
may affect venous circulation in some individuals.
What Happens When Vein Disease Develops
When vein valves become damaged, blood begins to move backward instead of upward.
This condition is known as venous reflux.
Venous reflux causes blood to accumulate in the lower legs, increasing pressure inside the veins.
Over time, this pressure can cause:
- enlarged veins
- swelling
- inflammation
- skin changes
Scientific research has explored how venous hypertension contributes to inflammation and vascular damage in chronic venous disease. One example of this research can be found in the PubMed database, which contains numerous studies on venous insufficiency and vascular inflammation:
https://pubmed.ncbi.nlm.nih.gov/29436147/
Common Symptoms of Vein Disease
Many people initially notice only visible veins, but symptoms often develop as the condition progresses.
Common symptoms include:
- leg heaviness
- aching legs
- swelling of the ankles or calves
- itching or burning sensations
- restless legs at night
- leg cramps during sleep
- fatigue in the legs after standing
Visible signs may include:
- spider veins
- bulging varicose veins
- skin discoloration around the ankles
In more advanced cases, chronic venous insufficiency can lead to venous ulcers, which are wounds that develop due to poor circulation.
Why Vein Disease Should Not Be Ignored
Many individuals assume that vein disease is only cosmetic.
However, untreated venous insufficiency may progressively worsen over time.
Complications may include:
- chronic swelling
- skin thickening
- discoloration
- venous ulcers
- increased risk of blood clots
Early diagnosis can often prevent these complications.
Modern Treatments for Vein Disease
Advances in medical technology have dramatically improved the treatment of vein disease.
Modern treatments are typically minimally invasive and performed in an outpatient setting.
Common treatment options include:
- endovenous laser therapy
- radiofrequency ablation
- ultrasound-guided sclerotherapy
- microphlebectomy
These treatments are designed to close dysfunctional veins so that blood can be redirected through healthier vessels.
Functional and Circulatory Health
While structural vein problems often require procedural treatment, overall vascular health is influenced by several lifestyle factors.
Supporting circulation may include:
- regular walking or exercise
- maintaining a healthy body weight
- avoiding prolonged sitting or standing
- elevating the legs when resting
Improving metabolic health and reducing inflammation may also support vascular function.
Vein Care in St. Louis
At Sheen Vein, we evaluate and treat patients throughout St. Louis, Clayton, Chesterfield, Arnold, and Farmington who are experiencing symptoms of venous disease.
Many patients initially seek care for cosmetic concerns such as spider veins, only to discover that underlying venous reflux is present.
Our goal is to help patients understand the circulatory nature of vein disease and develop personalized treatment strategies.
If you would like to learn more about vein conditions and treatment options, visit our website:
When to Seek Evaluation
You may benefit from a vein evaluation if you experience:
- leg heaviness or fatigue
- swelling in the ankles or calves
- visible varicose veins
- restless legs or leg cramps
- skin discoloration around the ankles
A vascular ultrasound can often determine whether venous reflux is present.
Final Thoughts
Vein disease is a common circulatory condition that affects millions of people.
Although genetics play a significant role, several factors—including aging, prolonged standing, pregnancy, and lifestyle—can contribute to the development of chronic venous insufficiency.
Research from institutions such as the Mayo Clinic, Cleveland Clinic, and studies indexed in PubMed continues to expand our understanding of how venous valve dysfunction and inflammation contribute to this condition.
Recognizing symptoms early and seeking evaluation can help prevent complications and improve quality of life.
For individuals in the St. Louis area, understanding the causes of vein disease is an important first step toward maintaining healthy circulation and addressing symptoms before they progress