What Is Photobiomodulation? Benefits, Uses, and How It Works

Light-based therapies have become increasingly popular in modern medicine and aesthetics because they offer non-invasive options for supporting healing and recovery.
One treatment gaining attention is photobiomodulation, which uses specific wavelengths of red or near-infrared light to stimulate cellular activity and encourage natural tissue repair. Many people searching online for “what is photobiomodulation” are looking for therapies that can help reduce inflammation, relieve pain, and improve overall tissue health without surgery.
Clinics such as Sheen Vein (Aesthetics and Functional Medicine) in St. Louis incorporate photobiomodulation into treatment programs that focus on both wellness and aesthetic care. This therapy is often used alongside other functional medicine approaches to help address issues such as musculoskeletal discomfort, recovery after physical strain, and skin rejuvenation.
By targeting cellular energy production, photobiomodulation treatments support the body’s natural healing processes while providing a comfortable, non-invasive treatment experience.
What Is Photobiomodulation?
Photobiomodulation (PBM) is a therapeutic technique that uses specific wavelengths of light to stimulate cellular processes in the body. The treatment typically involves red or near-infrared light delivered through medical devices.
This therapy works by stimulating mitochondria within cells. Mitochondria are responsible for producing ATP, the molecule that powers cellular activity.
When cells absorb light energy, several beneficial biological effects occur:
- Cellular metabolism increases, supporting tissue repair and regeneration
- Circulation improves, helping deliver oxygen and nutrients to injured areas
- Inflammation decreases, reducing pain and swelling in affected tissues
- Tissue repair processes become more active, supporting natural healing responses
Because of these effects, photobiomodulation is widely used in both medical and aesthetic treatments. Photobiomodulation is an important part of the clinical approach to pain management and functional recovery.
How Photobiomodulation Works
Photobiomodulation works at the cellular and mitochondrial level.
The treatment process typically follows these steps:
- Medical light wavelengths penetrate the skin and underlying tissues
- Cellular photoreceptors absorb the light energy
- Mitochondria respond by increasing ATP production, the energy source that powers cellular repair
- Cellular signaling pathways are activated, supporting regeneration and healing processes
At a biological level, this response helps reduce inflammation and supports the body’s natural ability to repair damaged or stressed tissue.
Key Benefits of Photobiomodulation
Photobiomodulation (PBM) therapy is a non-invasive light-based treatment that has been studied for its effects on cellular activity, inflammation, pain modulation, and tissue repair. It uses red or near-infrared light to interact with mitochondria, which are responsible for producing cellular energy (ATP).
1. Reduced Inflammation
Photobiomodulation has been studied for its ability to influence inflammatory pathways at the cellular level. It may help regulate oxidative stress and support improved microcirculation, which can contribute to reduced inflammation in soft tissues, joints, and muscles.
2. Pain Support
PBM is commonly used in clinical and rehabilitation settings for pain management. It has been investigated for conditions involving musculoskeletal discomfort, including muscle strain, joint stiffness, and back-related pain. The therapy is believed to influence nerve signaling and inflammatory responses that contribute to pain perception.
3. Tissue Repair and Healing Support
Photobiomodulation may support tissue repair by stimulating mitochondrial activity and increasing ATP production, which provides energy needed for cellular repair processes. Studies suggest PBM can enhance cell proliferation and support wound and soft tissue healing in various medical applications.
4. Skin Health Applications
In aesthetic and dermatological settings, PBM has been studied for its potential effects on skin quality.
It may support:
- collagen activity
- skin texture improvement
- overall skin regeneration processes
These effects are linked to increased cellular activity in fibroblasts, which play a role in collagen production.
5. Recovery After Physical Activity
Photobiomodulation is also used in sports and environmental rehabilitation to support recovery after physical exertion. It may help reduce delayed onset muscle soreness and support faster recovery by improving circulation and cellular energy availability.
Conditions Treated with Photobiomodulation
Photobiomodulation (PBM) therapy is a non-invasive light-based treatment that has been studied for its potential role in supporting recovery in a variety of musculoskeletal and soft tissue conditions. It is generally used as an adjunct therapy, meaning it supports but does not replace standard medical care such as rehabilitation, physical therapy, or medical management.
Musculoskeletal Pain
Musculoskeletal pain involves muscles, tendons, ligaments, and joints. PBM therapy has been studied for its potential to support pain reduction and tissue recovery by influencing cellular activity and inflammatory processes in affected tissues. Its use is most commonly explored in rehabilitation and pain management settings.
Back Pain
Back pain may result from muscle strain, postural stress, or degenerative changes. Research suggests that PBM may help support symptom relief in some cases of nonspecific back pain by modulating inflammation and promoting local tissue metabolism. It is typically used alongside other conservative treatments.
Plantar Fasciitis
Plantar fasciitis is an inflammatory and degenerative condition affecting the plantar fascia. Some clinical studies indicate that PBM may help reduce pain and support functional improvement by influencing local inflammation and tissue repair processes. However, results can vary depending on treatment parameters.
Sports Injuries
Sports-related injuries such as muscle strains, tendon irritation, and overuse injuries are common applications studied in PBM research. Evidence suggests PBM may support recovery by promoting cellular energy production (ATP), improving microcirculation, and modulating inflammation in soft tissues.
Why Patients Consider Photobiomodulation Therapy
Photobiomodulation (PBM) therapy is a non-invasive light-based treatment that some patients explore as an adjunct to conventional medical care, including medication, physical therapy, or other clinical interventions.
PBM is generally described in clinical literature as a low-risk, non-surgical modality that uses red or near-infrared light to interact with cellular processes. It does not involve incisions, drugs, or downtime typically associated with surgical procedures.
Commonly reported characteristics of PBM therapy include:
- non-invasive treatment approach
- minimal or no discomfort during application
- no surgical recovery period
- potential support for cellular and tissue repair processes
In clinical and research settings, PBM is being studied for its role in modulating inflammation and supporting recovery in musculoskeletal and soft tissue conditions. However, it is important to note that PBM is considered an adjunct therapy, meaning it is used to support, not replace, standard medical care.
FAQ Section
What does photobiomodulation do to the body?
Photobiomodulation stimulates mitochondria inside cells, increasing energy production and activating natural healing mechanisms.
Is photobiomodulation safe?
When performed by trained medical professionals, photobiomodulation therapy is generally considered safe and non-invasive.
How long does photobiomodulation treatment take?
Most sessions last between 10 and 30 minutes, depending on the treatment area.
What conditions can photobiomodulation treat?
PBM therapy is commonly used for musculoskeletal pain, sports injuries, plantar fasciitis, and back pain.
Does photobiomodulation hurt?
Most patients experience little to no discomfort during treatment.
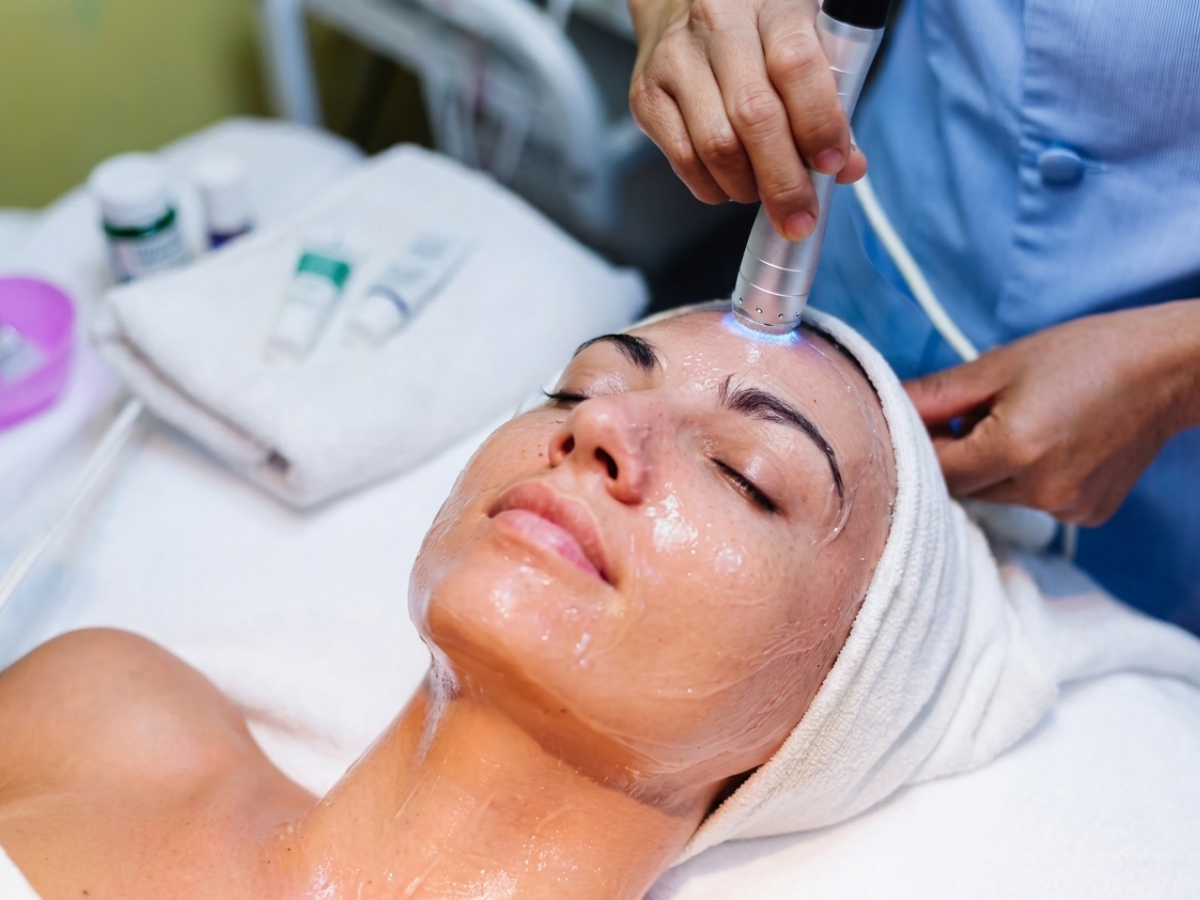
Understanding Photobiomodulation in Practice
Photobiomodulation therapy is a modern medical approach that uses light energy to stimulate healing, reduce inflammation, and support cellular repair. Because it is non-invasive and versatile, the therapy has become increasingly popular in both medical and aesthetic settings for individuals seeking supportive care for pain and recovery.
Individuals searching for what is photobiomodulation or photobiomodulation therapy near me can consult with specialists at Sheen Vein Aesthetics and Functional Medicine. The clinic provides advanced, non-invasive treatments designed to support recovery, improve wellness, and address pain-related conditions such as musculoskeletal discomfort and soft tissue injuries.
Scheduling a consultation allows patients to learn whether photobiomodulation therapy fits their individual health goals and determine if it can be integrated into a broader care plan focused on pain management and functional recovery.
Sheen Vein (Aesthetics and Functional Medicine)
11144 Tesson Ferry Rd #100, St. Louis, MO 63123
sheenveinandcosmetics.com
Plan Your Fat Transplant Journey
- Book Appointment – Schedule a consultation for photobiomodulation therapy options.
- Contact Now – Get more information about photobiomodulation therapy and personalized treatment options in St. Louis.